Employee Benefits
2026 Healthcare Cost Outlook | Cost Drivers & Trend Insights
2026 Healthcare Cost Outlook | Cost Drivers & Trend Insights
Most employers hoping for a reprieve in 2026 from escalating health care costs are finding themselves disappointed. Financial headwinds seem to be intensifying, with cost increases at their highest level in recent memory,1 exacerbating the challenge in managing budgets and affordability for employees. Per Brown & Brown’s “Employer Health and Benefits Strategy Survey – 2026 Edition,” employers ranked controlling cost for both themselves and their employees as their top two strategic priorities.
According to results from a recent Brown & Brown analysis, employers expect their healthcare costs to increase an average of 10% for 2026, after accounting for changes to their plan offerings (including plan design changes and types of plans being offered). If no changes were made to plan offerings, employers would have expected an increase of 12%.
Other industry segments are projecting elevated cost increases for 2026:
- Business Group on Health2 members expect a 9% increase in costs before plan changes
- Kaiser Family Foundation reports that insurers are raising premiums on public exchanges by an average of 26%3
- CMS announced that premiums for Medicare Part B coverage would be increasing by 9.7%4
- The International Foundation of Employee Benefit Plans anticipates a 10% increase in health care costs5
Employers are considering all options to manage their cost increases, including those that have been considered off the table in recent years. This includes offering limited network plans, raising copays, deductibles and coinsurance amounts, and excluding certain coverages.
The primary drivers of elevated cost trends over the past two to three years are expected to persist as the year continues. These include:
- Broad economic environment impacts
- Prescription drug costs
- Behavioral health utilization
- Large claimant volume increases
- Increasing prevalence of chronic diseases
However, there are newer headwinds emerging:
- No Surprises Act implications
- Hospitals’ increased emphasis on revenue cycle management
- New medical treatments and drugs coming to market
A Closer Look at Key Cost Drivers for Employers
Persistent Trends
1. Broader Economic Environment: Inflation & Labor Market
Healthcare providers have battled significant financial challenges since the onset of the COVID-19 pandemic, driven by the increased cost to deliver care. Provider burnout related to the pandemic and increased turnover has led to increased expenses for labor. These increased operating expenses for labor, supplies, and infrastructure have outpaced increases in reimbursement rates, leading providers to seek historically high increases to reimbursement rates. Concurrently, insurance carriers reported significant financial losses in 2024 and 2025. This environment results in contentious provider/ carrier contract negotiations.
Recent cuts to Medicaid will likely further strain hospitals’ financial outlook, with many forced to reduce services, close departments, or entire hospitals altogether in some rural geographies.6
Provider consolidation has also led to increased reimbursements, driven by additional market leverage gained via consolidation. Private equity-owned facilities and physician groups have also been associated with higher healthcare spend.
2. Prescription Drugs: GLP-1 and Biosimilars
Prescription drug costs continue to increase at a significantly higher rate than medical services. Unsurprisingly, GLP-1 drugs for weight loss are a constant topic of discussion around top cost drivers. GLP-1 utilization for weight loss skyrocketed in 2025, now representing over 20% of total prescription drug claims spend.7
Employers are grappling with determining the best way to cost-effectively provide access. Common tactics include limiting access to those meeting certain clinical criteria or requiring participation in lifestyle management programs.
Many carriers have begun excluding GLP-1s for weight loss from their fully-insured plans, with employers beginning to follow suit. What remains to be seen is how efforts to lower the list price of GLP-1s will cascade to employer-sponsored plans. Manufacturers have started to offer direct-to-consumer options at lower price points, allowing employers more flexibility in managing their population’s GLP-1 spend.
3. Behavioral Health
Behavioral health claims have a relatively small share of total claims (~10% of medical dollars). Nevertheless, behavioral health claims have increased by 17% in 2025,8 and some employers have seen the category emerge in their top five spend areas. Behavioral health patients also tend to have other co-morbidities exacerbating claims spend. More than half of patients with a high-cost condition also have a behavioral health disorder, and behavioral health disorders lead to increased medical spending for chronic pain, cardiovascular disease, and diabetes.9
Historically, out-of-network substance use disorder programs accounted for a significant share of claims spending. Recently, the primary cost driver has shifted to a surge in high-frequency, low-severity visits (outpatient therapy). This benefit continues to gain traction with younger generations, and as a result, many carriers have been expanding their network to address access issues. This network expansion, however, will likely lead to higher reimbursements to providers, further pressuring the broader unit cost inflation.
4. Increasing Volume of Large Claimants
The volume of large claimants has increased dramatically in the post-pandemic period, not just truly catastrophic million dollar claimants, but those that would not reach typical stop-loss thresholds. The number of claimants incurring $100,000 (per 1,000 members) increased 14% in 2025,10 while the average cost per claimant remained stable over this same period. This increase in the number of large claimants can be explained by several components, including a higher prevalence of chronic conditions, more costly treatments (e.g., gene therapies), new technology, and an aging population.
5. Prevalence of Chronic Diseases
Chronic diseases, such as hyperlipidemia, hypertension, obesity, and diabetes, are the leading cause of illness and death in the United States and represent over 90% of overall medical spending.11 Per a recent FAIR Health report, nearly 60% of patients were treated for at least one chronic condition. For those with at least one chronic condition, the average number of conditions was three. The average cost of a member without any chronic conditions was $1,590 in 2024 – whereas the average cost for someone with three chronic conditions was nearly $5,000.12
Emerging Trends
No Surprises Act Implications
One of the goals of the No Surprises Act was to protect patients from unexpected medical bills, particularly from providers for whom they would not be aware of network status (such as anesthesiologists and radiologists). The law established an arbitration process called Independent Dispute Resolution (IDR) to address payment disputes between out-of-network providers and payers.
When first created, CMS initially expected 17,000 disputes to be submitted. Within nine months, approximately 190,000 disputes had been filed, and the backlog quickly grew to over 500,000. A high proportion of submissions have been made by a relatively small percentage of providers, primarily by private equity-backed groups. Providers have also won over 85% of disputes and plan sponsors ultimately paid fees that are three to four times typical in-network rates.13 The high volume of disputes generates higher spending, which will ultimately cascade into higher plan costs.
Hospitals’ Increased Emphasis on Revenue Cycle Management
As mentioned, hospitals’ finances have been strained for the last several years, with most only having the opportunity to renegotiate reimbursement rates every few years. In the interim, hospital systems have been working to optimize revenue streams under existing rates. Historically, providers have lagged insurers in leveraging technology to streamline administrative and billing tasks. New revenue cycle management companies have emerged to offer automated, AI-enhanced solutions. These solutions would result in hospitals collecting higher revenue, which, in turn, would result in higher costs for insurers and self-funded employer-sponsored plans.
Changes in coding has also been observed since early 2024, with utilization of higher intensity services (and higher reimbursement rates) increasing dramatically.14
New Medical Treatments and Drugs Coming to Market
Cellular and gene therapies are increasingly providing innovative treatments for a growing number of rare and previously untreatable diseases. While the incidence rates for these treatments is currently very low, the cost per treatment can be astronomically high – list prices for recently approved drugs are over $2-3 million for one-time infusions. Medical carriers are able to manage the risk by spreading anticipated costs over their entire book of business, but employers do not have that luxury when budgeting for annual plan costs.
Conclusion
Employers should approach their strategy work and budget-setting process over the next few years, assuming the current financial headwinds persist, driven by a challenging economic environment and the newer, emerging trends. By taking proactive action and working with carriers, pharmacy benefit managers, and advisors, employers can position themselves to manage these emerging risks within their broader health plan strategy. Employers should push their vendors to share more detailed data on a more timely basis to help better forecast emerging cost drivers, monitor and actively manage the areas described above, and course correct as necessary.
Brown & Brown Employer Health and Benefits Strategy Survey – Findings
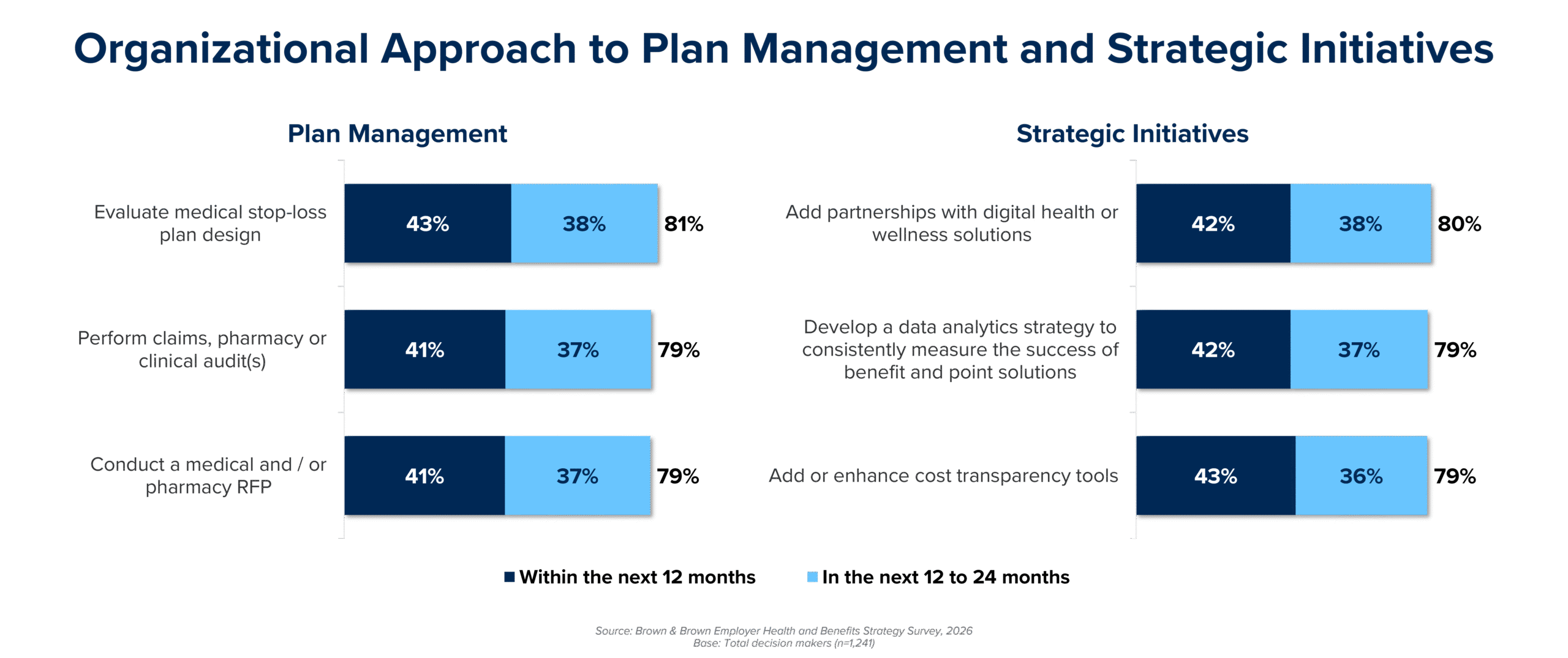
Controlling both employer and employee costs continues to be a top priority for employers in 2026 and beyond. To navigate and mitigate the financial challenges of rising costs, employers are actively exploring a range of plan management and strategic initiatives over the next 12-24 months (as shown in exhibit below).
- The leading plan management initiatives for employers is evaluating medical stop-loss plan designs (81%) and conducting medical and/or pharmacy RFPs (79%). Another top priority is conducting audits (79%) across medical, pharmacy and clinical programs as a best practice to uphold fiduciary responsibilities and ensure the integrity and compliance of their health plans.
- The momentum for introducing virtual and digital health solutions is another popular strategy (80%), as they increasingly become a fundamental component of employee health benefits.
1 https://www.wsj.com/health/healthcare/health-insurance-costs-rise-6cc1b934
2 https://www.businessgrouphealth.org/resources/2026-employer-health-care-strategy-survey-executive-summary
3 https://www.kff.org/quick-take/aca-insurers-are-raising-premiums-by-an-estimated-26-but-most-enrollees-could-see-sharper-increases-in-what-they-pay/
4 https://www.cms.gov/newsroom/fact-sheets/2026-medicare-parts-b-premiums-deductibles
5 https://www.ifebp.org/resources—news/news-and-regulatory-updates/press-room/press-releases/2025/08/14/employers-project-10–rise-in-health-care-costs-for-2026
6 https://www.bostonglobe.com/2025/12/01/business/massachusetts-hospitals-medicaid-cuts/
7,8,10 Brown & Brown Claims Data Warehouse analysis
9 https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2829859
11 https://www.cdc.gov/chronic-disease/data-research/facts-stats/index.html
12 FAIR Health, “Chronic Conditions in the United States – A Study of Commercial Claims”
13 https://www.healthaffairs.org/content/forefront/substantial-costs-no-surprises-act-arbitration-process
14 UnitedHealthcare analysis

Kevin Baker, FSA, MAAA, FCA
Principal